|
What is Dementia?
Dementia is a general term for a decline in mental ability severe enough to interfere with daily life. Dementia is not a specific disease. It's an overall term that describes a group of symptoms associated with a decline in memory or other thinking skills severe enough to reduce a person's ability to perform everyday activities. Alzheimer's disease accounts for 60 to 80 percent of cases. There are many other conditions that can cause symptoms of dementia, including some that are reversible, such as thyroid problems and vitamin deficiencies. Symptoms While symptoms of dementia can vary greatly, at least two of the following core mental functions must be significantly impaired to be considered dementia:
What causes dementia? Dementia is caused by damage to brain cells. This damage interferes with the ability of brain cells to communicate with each other. When brain cells cannot communicate normally, thinking, behaviour and feelings can be affected. While most changes in the brain that cause dementia are permanent and worsen over time, thinking and memory problems caused by the following conditions may improve when the condition is treated or addressed: depression, medication side effects, excess use of alcohol, thyroid problems, vitamin deficiencies. Diagnosis of dementia There is no one test to determine if someone has dementia. Doctors diagnose Alzheimer's and other types of dementia based on a careful medical history, a physical examination, laboratory tests, and the characteristic changes in thinking, day-to-day function and behaviour associated with each type. Doctors can determine that a person has dementia with a high level of certainty. Dementia treatment and care Treatment of dementia depends on its cause. In the case of most progressive dementias, including Alzheimer's disease, there is no cure and no treatment that slows or stops its progression. But there are drug treatments that may temporarily improve symptoms. The same medications used to treat Alzheimer's are among the drugs sometimes prescribed to help with symptoms of other types of dementias. Non-drug therapies can also alleviate some symptoms of dementia. How Alzheimer's medications work To understand how Alzheimer's medications work, you first need to understand the communication network in the brain. The picture below depicts nerve cells, or neurons, in the brain. Neurons are the chief cells destroyed by Alzheimer's disease. In the brain, neurons connect and communicate at synapses, where tiny bursts of chemicals called neurotransmitters carry information from one cell to another. Alzheimer's disrupts this process, and eventually destroys synapses and kills neurons, damaging the brain's communication network. As Alzheimer’s progresses, brain cells die and connections among cells are lost, causing cognitive symptoms to worsen. While current medications cannot stop the damage Alzheimer’s causes to brain cells, they may help lessen or stabilize symptoms for a limited time by affecting certain chemicals involved in carrying messages among the brain's nerve cells. Overview of disease progression The symptoms of Alzheimer's disease worsen over time. On average, a person with Alzheimer's lives four to eight years after diagnosis, but can live as long as 20 years, depending on other factors. Changes in the brain related to Alzheimer's begin years before any signs of the disease. This time period, which can last for years, is referred to as preclinical Alzheimer's disease. Mild Alzheimer's disease (early stage) In the early stage of Alzheimer's, a person may function independently. He or she may still drive, work and be part of social activities. Despite this, the person may feel as if he or she is having memory lapses, such as forgetting familiar words or the location of everyday objects. Friends, family or others close to the individual begin to notice difficulties. Common difficulties include:
Moderate Alzheimer's disease (middle stage) During the moderate stage of Alzheimer’s, the dementia symptoms are more pronounced. A person may have greater difficulty performing tasks, such as paying bills, but they may still remember significant details about their life. You may notice the person with Alzheimer's confusing words, getting frustrated or angry, or acting in unexpected ways, such as refusing to bathe. Damage to nerve cells in the brain can make it difficult to express thoughts and perform routine tasks. At this point, symptoms will be noticeable to others and may include:
In the final stage of this disease, dementia symptoms are severe. Individuals lose the ability to respond to their environment, to carry on a conversation and, eventually, to control movement. They may still say words or phrases, but communicating pain becomes difficult. As memory and cognitive skills continue to worsen, significant personality changes may take place and individuals need extensive help with daily activities. At this stage, individuals may:
Top of Form Daily Care A person living with dementia will eventually need assistance with daily living. By using creativity and caregiving skills, you can adapt routines and activities as needs change. Use our resources to get ideas and connect with other caregivers. Examples of different aspects on assisting a person with dementia in caregiving: A daily Care Plan, activities of daily living, communication and Alzheimers, incontinence, bathing, dressing and grooming, dental care, treatments, medication safety, working with the doctor, adequate food and fluid intake, care of bowel and bladder function, skin and body health, infections and pneumonia, pain and illness The role of a caregiver During the late stages, the role as a caregiver focuses on preserving quality of life and dignity. Although a person in the late stage of Alzheimer's typically loses the ability to talk and express needs, research tells us that some core of the person's self may remain. This means you may be able to continue to connect throughout the late stage of the disease. At this point in the disease, the world is primarily experienced through the senses. Express caring through touch, sound, sight, taste and smell. Dementia help and support is available Since care needs are extensive during the late stage, they may exceed what you can provide at home, even with additional assistance. This may mean moving the person into a facility in order to get the care needed. Deciding on late-stage care can be one of the most difficult decisions families face. Families that have been through the process tell us that it is best to gather information and move forward, rather than second guessing decisions after the fact. There are many good ways to provide quality care. Remember, regardless of where the care takes place, the decision is about making sure the person receives the care needed. At the end of life, another option is hospice. The underlying philosophy of hospice focuses on quality and dignity by providing comfort, care and support services for people with terminal illnesses and their families. Ideally, discussions about end-of-life care wishes should take place while the person with the dementia still has the capacity to make decisions and share wishes about life-sustaining treatment. References The information was extracted from the following sites: https://www.alz.org/alzheimers-dementia/what-is-dementia http://www.neuropsychologysa.co.za/support-groups/alzheimers-south-africa-support-groups/ Other sites with helpful information on local care and support: https://www.newseveryday.co.za/news/online-dementia-support-group This is a South African Facebook support group that aims to provide a safe and accessible space for families and individuals impacted by dementia KwaZulu-Natal 031-702 4321: Support groups Amanzimtoti, Durban (Berea), Durban North, Hillcrest, Howick, KwaNgcolosi, Lower Molweni, Musgrave, Newcastle, Pietermaritzburg, Pinetown, Port Shepstone, Scottburgh, Umbilo, Upper Molweni, Vryheid The Vales Care Centre Pennington : 039 975 1337 or email val@vales.co.za Meningococcal meningitis
Summary:
Meningitis is an infection of the meninges, the thin lining that surrounds the brain and the spinal cord. Several different bacteria, viruses, fungi and some drugs and medical conditions i.e. inflammatory diseases such as lupus can cause meningitis. Neisseria meningitidis is one of the most important because of its potential to cause epidemics. Meningococcal meningitis is caused by Neisseria meningitidis bacteria. Transmission
The diagnosis of meningococcal meningitis is suspected by the clinical presentation and a lumbar puncture showing a purulent spinal fluid. Sometimes the bacteria can be seen in microscopic examinations of the spinal fluid. The diagnosis is confirmed by growing the bacteria from specimens of spinal fluid or blood. Epidemiology Meningitis in South Africa has sporadic outbreaks, which are most prevalent during droughts, dry and dusty or winter seasons. The number of cases increases in winter and spring. During the dry season, between December and June, because of dust winds and upper respiratory tract infections due to cold nights, the local immunity of the pharynx is diminished increasing the risk of meningitis. At the same time, the transmission of N. meningitidis is favoured by overcrowded housing at family level and by large population displacements due to pilgrimages and traditional markets at regional level. Treatment
Prophylaxis Currently recommendations for chemoprophylaxis in South Africa are as follows:
Vaccines are available to prevent the disease.
References: www.kznhealth.gov.za/meningitis.htm https://www.who.int/news-room/fact-sheets/detail/meningococcal-meningitis Headaches are one of the most common medical complaints that we see in family practice. Most people experience them at some point in their life. They can affect anyone regardless of age, race, and gender.
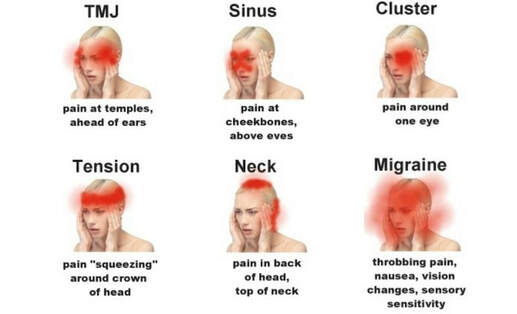
A headache can be a sign of stress or emotional distress, or it can result from a medical disorder, such as migraine or high blood pressure, anxiety, or depression. It can lead to other problems. People with chronic migraine headaches, for example, may find it hard to attend work or school regularly. Primary headaches Primary headaches are stand-alone illnesses caused directly by the overactivity of, or problems with, structures in the head that are pain-sensitive. This includes the blood vessels, muscles, and nerves of the head and neck. They may also result from changes in chemical activity in the brain. Common primary headaches include migraines, cluster headaches, and tension headaches. Secondary headaches Secondary headaches are symptoms that happen when another condition stimulates the pain-sensitive nerves of the head. In other words, the headache symptoms can be attributed to another cause. A wide range of different factors can cause secondary headaches. These include: · alcohol-induced hangover · brain tumor · blood clots · bleeding in or around the brain · "brain freeze," or ice-cream headaches · carbon monoxide poisoning · concussion · dehydration · glaucoma · teeth-grinding at night · influenza · overuse of pain medication, known as rebound headaches · panic attacks · stroke As headaches can be a symptom of a serious condition, it is important to seek medical advice if they become more severe, regular, or persistent. For example, if a headache is more painful and disruptive than previous headaches, worsens, or fails to improve with medication or is accompanied by other symptoms such as confusion, fever, sensory changes, and stiffness in the neck, a doctor should be contacted immediately. Types Tension headaches Tension headaches are the most common form of primary headache. Such headaches normally begin slowly and gradually in the middle of the day. The person can feel: · as if they have a tight band around the head · a constant, dull ache on both sides · pain spread to or from the neck Tension-type headaches can be either episodic or chronic. Episodic attacks are usually a few hours in duration, but it can last for several days. Chronic headaches occur for 15 or more days a month for a period of at least 3 months. Migraines A migraine headache may cause a pulsating, throbbing pain usually only on one side of the head. The aching may be accompanied by: · blurred vision · light-headedness · nausea · sensory disturbances known as auras Migraine is the second most common form of primary headache and can have a significant impact on the life of an individual. According to the WHO, migraine is the sixth highest cause of days lost due to disability worldwide. A migraine can last from a few hours to between 2 and 3 days. Rebound headaches Rebound or medication-overuse headaches stem from an excessive use of medication to treat headache symptoms. They are the most common cause of secondary headaches. They usually begin early in the day and persist throughout the day. They may improve with pain medication, but worsen when its effects wear off. Along with the headache itself, rebound headaches can cause: · neck pain · restlessness · a feeling of nasal congestion · reduced sleep quality Rebound headaches can cause a range of symptoms, and the pain can be different each day. Cluster headaches Cluster headaches usually last between 15 minutes and 3 hours, and they occur suddenly once per day up to eight times per day for a period of weeks to months. In between clusters, there may be no headache symptoms, and this headache-free period can last months to years. The pain caused by cluster headaches is: · one-sided · severe · often described as sharp or burning · typically located in or around one eye The affected area may become red and swollen, the eyelid may droop, and the nasal passage on the affected side may become stuffy and runny. Thunderclap headaches These are sudden, severe headaches that are often described as the "worst headache of my life." They reach maximum intensity in less than one minute and last longer than 5 minutes. A thunderclap headache is often secondary to life-threatening conditions, such as intracerebral hemorrhage, cerebral venous thrombosis, ruptured or unruptured aneurysms, reversible cerebral vasoconstriction syndrome (RVS), meningitis, and pituitary apoplexy. who experience these sudden, severe headaches should seek medical evaluation immediately. Headaches in children Importantly, in children and adolescents, primary headaches are often co-morbid with psychiatric conditions. Awareness of, and enquiry about, sleep disorders, PTSD, school phobias, ADHD, conduct disorder, learning disorders, encopresis (soiling of underwear with stool past the age of toilet training), enuresis (bedwetting), depression and anxiety is important when assessing a child with headaches. Treatment The most common ways of treating headaches are rest and pain relief medication. Generic pain relief medication is available over the counter (OTC), or doctors can prescribe preventative medication, such as tricyclic antidepressants, serotonin receptor agonists, anti-epilepticdrugs,andbeta-blockers. It is important to follow the doctor's advice because overusing pain relief medication can lead to rebound headaches. The treatment of rebound headaches involves the reducing or stopping pain relief medication. In extreme cases, a short hospital stay may be needed to manage withdrawal safely and effectively. Alternative treatments Several alternative forms of treatment for headaches are available, but it is important to consult a doctor before making any major changes or beginning any alternative forms of treatment. Alternative approaches include: · acupuncture · cognitive behavior therapy · hypnosis · meditation Research has not provided evidence to confirm that all these methods work. Sometimes, a headache may result from a deficiency of a particular nutrient or nutrients, especially magnesium and certain B vitamins. Nutrient deficiencies can be due to a poor quality diet, underlying malabsorption issues, or other medical conditions. Home remedies A number of steps can be taken to reduce the risk of headaches and to ease the pain if they do occur: 1. Apply a heat pack or ice pack to your head or neck, but avoid extreme temperatures. 2. Avoid stressors, where possible, and develop healthy coping strategies for unavoidable stress. 3. Eat regular meals, taking care to maintain stable blood sugar. A hot shower can help, although in one rare condition hot water exposure can trigger headaches. Exercising regularly and getting enough rest and regular sleep contributes to overall health and stress reduction. Diagnosis A doctor will usually be able to diagnose a particular type of headache through a description of the condition, the type of pain, and the timing and pattern of attacks. If the nature of the headache appears to be complex, tests may be carried out to eliminate more serious causes. Further testing could include: · blood tests · X-rays · brain scans, such as CT and MRI The WHO points out that headaches are often not taken seriously because they are sporadic, most headaches do not lead to death, and they are not contagious. References:
|
AuthorYour SFC doctors ArchivesCategories |